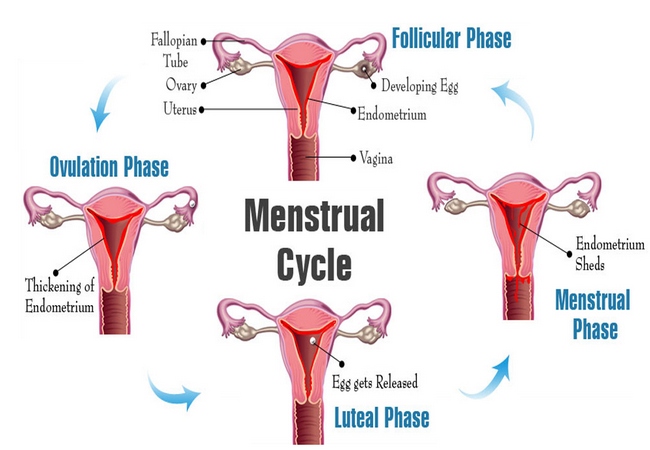
Endometrial Changes During Menstrual Cycle Phases
What Do You Mean by Menstruation?
Menstruation, or period, is normal vaginal bleeding that occurs as part of a woman’s monthly cycle. Every month, your body prepares for pregnancy. If no pregnancy occurs, the uterus, or womb, sheds its lining. The menstrual blood is partly blood and partly tissue from inside the uterus. It passes out of the body through the vagina.
Periods usually start between age 11 and 14 and continue until menopause at about age 51. They usually last from three to five days. Besides bleeding from the vagina, you may have.
- Abdominal or pelvic cramping pain,
- Lower back pain,
- Bloating and sore breasts,
- Food cravings,
- Mood swings and irritability,
- Headache and fatigue.
Premenstrual syndrome, or PMS, is a group of symptoms that start before the period. It can include emotional and physical symptoms.
You can read: Pregnancy Sign, Symptoms and Confirmation Test
What is Menstrual Cycle?
The cyclical changes in the female that takes place in the endometrium and results in bleeding per vagina from uterus is called menstrual cycle.
The female menstrual cycle includes the cycle of regular changes in: the anterior pituitary gland hormones, in the ovaries, and in the uterine endometrial lining. These changes are designed to prepare the woman’s body for possible pregnancy.

The hormonal cycle of hypothalamus and anterior pituitary gland – hormones include: gonadotrophin releasing hormone (GnRH), oestrogen, progesterone, follicle stimulating hormone (FSH) and luteinising hormone (LH).
- Hypothalamus produces GnRH;
- This influences the anterior pituitary gland to secrete FSH and LH;
- Gonadotrophic activity of hypothalamus and anterior pituitary gland influenced by feedback mechanisms from ovarian hormones.
- FSH causes Graafian follicles in ovaries to develop and enlarge, and secrete oestrogen;
- LH is produced a few days after FSH, caused by rising oestrogen levels;
- After ovulation, levels of FSH and LH drop rapidly;
- Progesterone inhibits any new rise in LH;
- If no pregnancy, corpus luteum degenerates after 14 days;
- Negative feedback mechanism of progesterone stops, so FSH and LH can rise again and new cycle begins.
The ovarian cycle includes – follicular phase, ovulatory phase, and luteal phase.
- Graafian follicle – under influence of FSH and later LH, this matures, moves to surface of ovary and
- Ruptures to release ovum (ovulation);
- The empty follicle is known as corpus luteum, which collapses and atrophies unless pregnancy occurs.
The uterine or endometrial cycle includes- proliferative phase, secretory phase, and menstrual phase.
- Following menstruation until ovulation the endometrium regenerates ((proliferates) and thickens, under influence of oestrogen;
- Secretory phase follows ovulation, under influence of progesterone and oestrogen from corpus luteum; the functional layer of endometrium thickens and becomes spongy because of the numerous glands;
- Menstrual phase, where if pregnancy has not occurred, the thickened endometrium is shed as vaginal bleeding.
There are also changes in the cervical mucous.
Endometrial Changes in Menstrual Cycle Phases:
Cycle has been traditionally divided into three phases:
- Menstrual phase: The first 4 days
- Proliferative phase: 10 days
- Secretary phase: 14 days
All the above three phases have discussed in the below:
1. Menstrual Phase:
As a result of the ovarian cycle the uterus is subjected to the influence first of oestrogen and then of a combination of oestrogen and progesterone. Both are withdrawn when the corpus luteum degenerates and menstruation occurs within a few days. The concentration of the estrogen & progesterone fall leading to changes in local prostaglandin metabolism & concentration.
Many of the arterioles show intense vaso-constriction & some of the called arterioles become kinked, as the endometrium shrinks, there is stasis of blood flow in them. From time to time ,some of the arterioles relax & bleeding occurs through the necrosed walls of the vessels in the functional layer of the endometrium leads to its disintegration.
2. Proliferative Phase:
(Folicular phase/ oestrogenic phase/ postmenstrual phase/ Preovulatory phase): After menstruation only the stratum basalis is left. Under the influence of oestrogen from the ripening follicle, the cells of the surface epithelium& glands become taller & more columnar. The glands which are at first straight, narrow and tubular gradually Wingate and widen becoming slightly tortuous. The stromal cells hypertrophy.
Two types of blood vessels are seen in the endometrium: Short straight in the basal layer and long coiled areoles into the functional layer; Endometrium measures 2-3 mm.
3. Secretary Phase:
(Luteal phase, progesteronic or post ovulatory or premenstrual phase)
After ovulation the corpus luteum seretes both estrogen & progesterone. Under influence of these hormones’ glands become extremely tortuous & their epithelium projects into their lumina. Hypertrophy of the stromal cells continues until they resemble the decidual cells or pregnancy.
You can read: Effect of Menstrual Cycle on Breastfeeding
Theendrometrium becomes 5-7 mm thick and shows three layers:
- In the stratum compactum, the stromal cells are closely packed and the necks of the glands are straight.
- In the stratum spongiosum convoluted glands coiled arterioles & comparatively few stromal cells.
- An inactive basal layer which shows little secretory response. This is not shed during menstruation.
More questions related to this article:
- What is menstruation?
- Define menstruation.
- What is menstrual cycle?
- What do you mean by menstrual cycle?
- Describe the endometrial change in different stages of menstrual cycle.
- Mention phases of menstruation with duration.